Turn your transportation benefit into a STAR rating advantage
One-third of Medicare beneficiaries miss or delay care because of transportation barriers. For MA plans, that means avoidable care gaps, lower STAR scores, and preventable member churn. Ride Health turns your supplemental transportation benefit into a strategic asset.
The Strategic Case for NEMT in MA
Transportation is not just a supplemental benefit. It is a measurable quality lever that touches care access, member experience, and plan economics.
Every dollar invested in NEMT returns up to eleven dollars in avoided downstream medical costs through reduced ER visits, hospital readmissions, and delayed care escalation.
One-third of Medicare beneficiaries miss or delay care due to transportation barriers, directly impacting HEDIS measures and STAR performance.
Multiple HEDIS measures track access to care, and transportation is a recognized barrier. Plans that address NEMT systematically close care gaps faster.
CMS increasingly incorporates social determinants of health into quality measurement. Transportation is one of the most actionable SDOH levers available to plans.
In a crowded MA market, a well-executed transportation benefit is a tangible differentiator that members experience directly and factor into plan selection and retention.
Purpose-built for complex ride coordination
Every detail about a passenger — mobility, communication, behavioral needs — shapes how rides are planned and executed.
1 / 3
Create Ride — Setup
Configure ride details, assign passengers from your roster, and set pickup/drop-off locations in a single streamlined workflow.
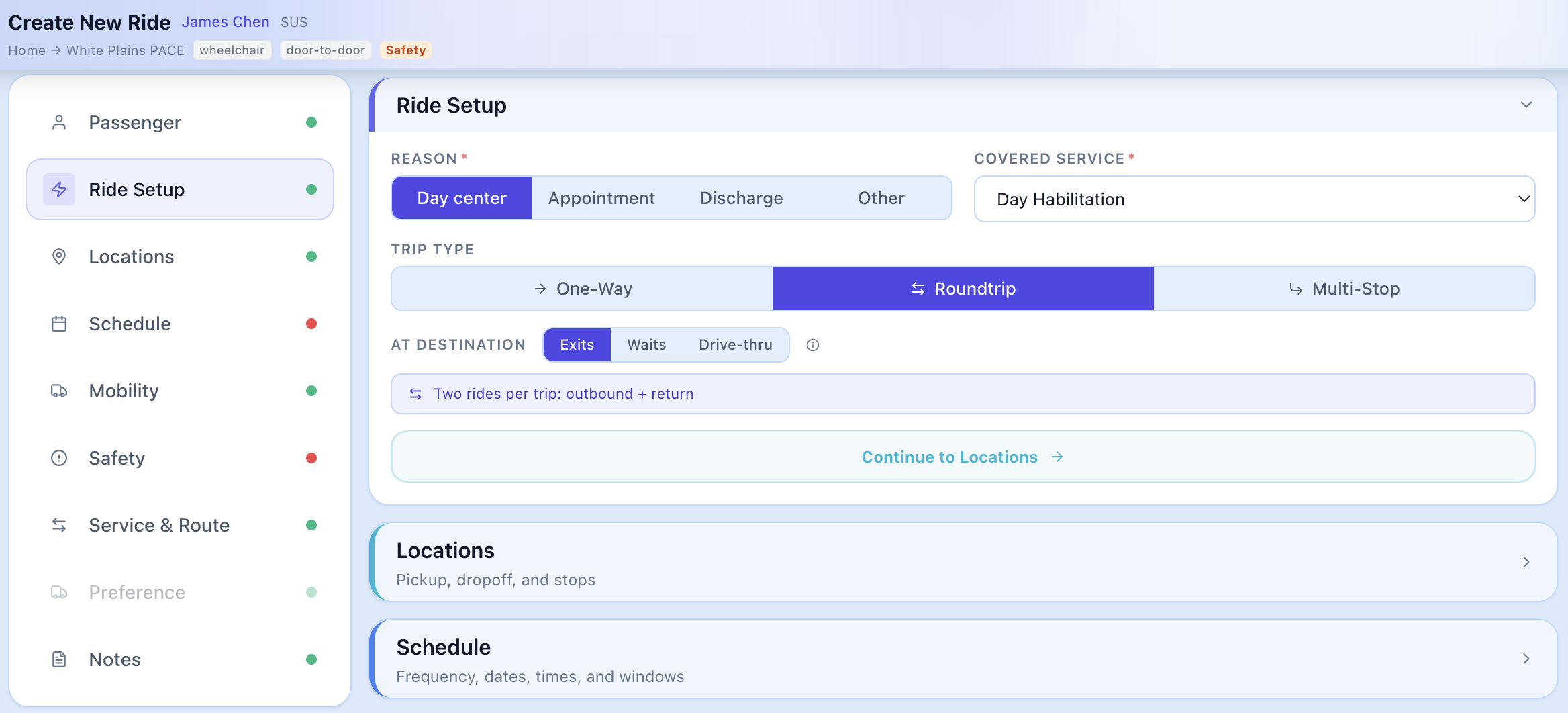
Three Ways to Set Your Plan Apart
Ride Health helps Medicare Advantage plans compete on quality, experience, and retention through purpose-built transportation operations.
Close Care Gaps
Proactively identify members with transportation barriers and connect them to rides before appointments are missed. Target high-value visits for chronic disease management, preventive screenings, and post-discharge follow-ups to improve HEDIS completion rates.
Improve STAR Measures
Align transportation operations with the specific HEDIS and CAHPS measures that drive STAR ratings. Track ride completion against quality targets and surface actionable data to care management teams so transportation supports rather than undermines your quality strategy.
Retain Members
Deliver a transportation experience that members notice and value. On-time performance, rider-friendly scheduling, and consistent quality drive higher satisfaction scores and reduce the likelihood of members switching plans during AEP.
What Ride Health Delivers
A complete NEMT solution designed for the operational, compliance, and quality requirements of Medicare Advantage plans.
Benefit Configuration
Flexible benefit design supporting ride caps, dollar limits, service-type restrictions, and authorization workflows that mirror your plan's supplemental benefit structure.
Member Scheduling
Multiple booking channels including phone, web portal, and care manager referral so members and their caregivers can access rides through the channel that works best for them.
Quality-Aligned Reporting
Dashboards and reports that map transportation utilization and outcomes directly to HEDIS measures, STAR domains, and member satisfaction metrics your quality team tracks.
Network Adequacy
A managed network of vetted transportation providers with the vehicle types, service levels, and geographic coverage to meet access standards across your plan's service area.
FWA Prevention
Built-in fraud, waste, and abuse controls including trip verification, mileage validation, and anomaly detection to protect your plan and satisfy CMS compliance requirements.
