Transportation that matches the complexity of your members
MLTC and MLTSS members have the highest transportation needs and the most complex requirements. Ride Health is built to manage that complexity at scale — with the operational rigor your regulators and members expect.
- Benefit-aware — configurable rules for dual eligibility and authorization
- Operationally rigorous — 24/7 contact center with trained, multilingual agents
- Regulatory-ready — pre-built reporting for state MLTC/MLTSS requirements
Why MLTC/MLTSS Transportation Is Uniquely Complex
Managing transportation for long-term care members requires capabilities that go far beyond basic ride scheduling. Every dimension — clinical, operational, regulatory, and financial — adds complexity.
Dual Eligibility & Benefit Layering
Members may have overlapping Medicare and Medicaid transportation benefits with different rules, limits, and authorization requirements that must be managed simultaneously.
High Ride Volume & Frequency
MLTC/MLTSS members often need daily or multi-weekly transportation to adult day programs, dialysis, behavioral health, and other recurring services — generating thousands of rides per month.
Complex Mobility & Medical Needs
Wheelchair users, stretcher transport, bariatric needs, oxygen dependency, and behavioral considerations require specialized vehicles and trained drivers for every ride.
State-Specific Regulations
Each state has unique MLTC/MLTSS reporting requirements, quality standards, grievance processes, and network adequacy rules that transportation operations must satisfy.
Communication Challenges
Members and caregivers may have limited English proficiency, hearing or vision impairments, or cognitive limitations that require multilingual, multi-channel communication strategies.
Purpose-built for complex ride coordination
Every detail about a passenger — mobility, communication, behavioral needs — shapes how rides are planned and executed.
1 / 3
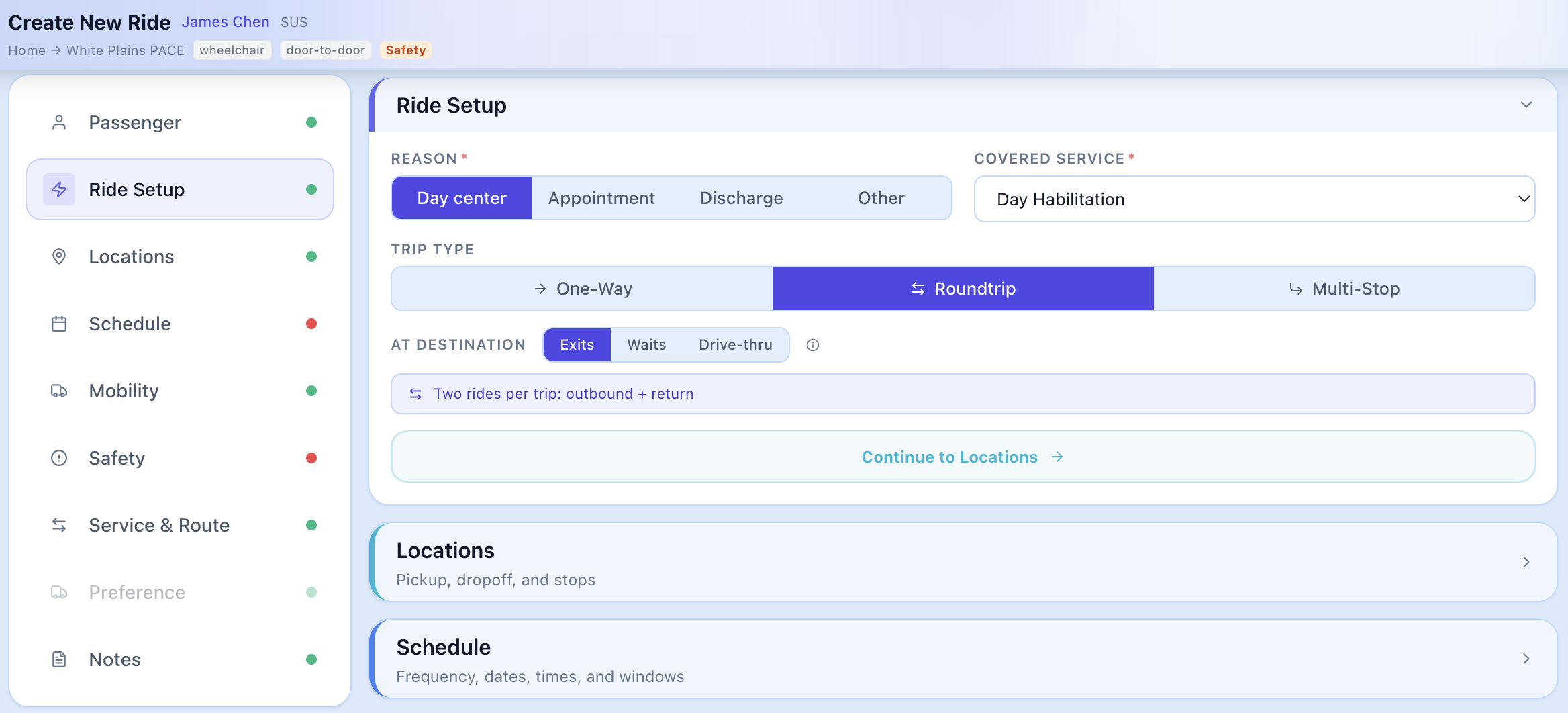
Create Ride — Setup
Configure ride details, assign passengers from your roster, and set pickup/drop-off locations in a single streamlined workflow.
What Ride Health Delivers
A complete transportation benefit management solution designed for the operational, regulatory, and member-experience demands of MLTC and MLTSS programs.
Benefit Management
Configure transportation benefits by plan type, eligibility category, and service authorization — with automated utilization tracking, limit enforcement, and prior authorization workflows.
Roster Integration
Automated member roster syncing with eligibility verification, enrollment/disenrollment processing, and benefit assignment based on plan configuration.
Hybrid Fulfillment
Route rides across contracted providers, community transit, and on-demand networks using configurable rules that balance cost, quality, vehicle type, and member preference.
Omni-Channel Contact Center
A 24/7/365 contact center staffed by trained agents who handle ride scheduling, changes, complaints, and escalations via phone, SMS, email, and web — in multiple languages.
FWA Prevention
Automated fraud, waste, and abuse detection including duplicate ride identification, GPS trip verification, unusual utilization pattern alerts, and provider billing validation.
Regulatory Reporting
Pre-built and custom reports aligned with state MLTC/MLTSS requirements including grievance tracking, quality metrics, network adequacy documentation, and encounter data.
Alignment with Plan Operations
Transportation does not operate in a silo. Ride Health integrates with your plan's care management, compliance, provider network, and financial operations.
Care Management Integration
Transportation data flows into care management workflows — ride completion, missed trips, and member behavior patterns that inform care planning and risk stratification.
Grievance & Appeals
Integrated grievance tracking with root cause analysis, resolution workflows, and regulatory-compliant documentation and reporting timelines.
Provider Network Management
Credentialing, performance scorecards, rate management, and capacity monitoring for every transportation provider in your network.
Financial Reconciliation
Automated trip verification, invoice reconciliation, and cost reporting by member, plan, service category, and provider — with full audit trails.
